DR WILLIAM MOONEY
Sydney Specialty ENT Surgeon with Rhinoplasty Experience
AHPRA specialist registration MED0001145166
Specialising in some of the most complicated and intricate forms of rhinoplasty (nose) surgery. Dr Mooney is a fully qualified ENT surgeon. After becoming a Fellow of the Royal Australasian College of Surgeons, Dr Mooney completed formal training Fellowships in rhinology and head and neck surgery at the Royal National Throat, Nose and Ear Hospital, London and the Facial Plastic and Cosmetic Fellowship with the Australian Academy of Facial Plastic Surgeons. He has attended visiting fellowships in further facial cosmetic surgery at the Lasky Clinic, Los Angeles, head and neck surgery at Memorial Sloan Kettering New York, and Voice pathology and surgery with Jean Abitol in Paris.
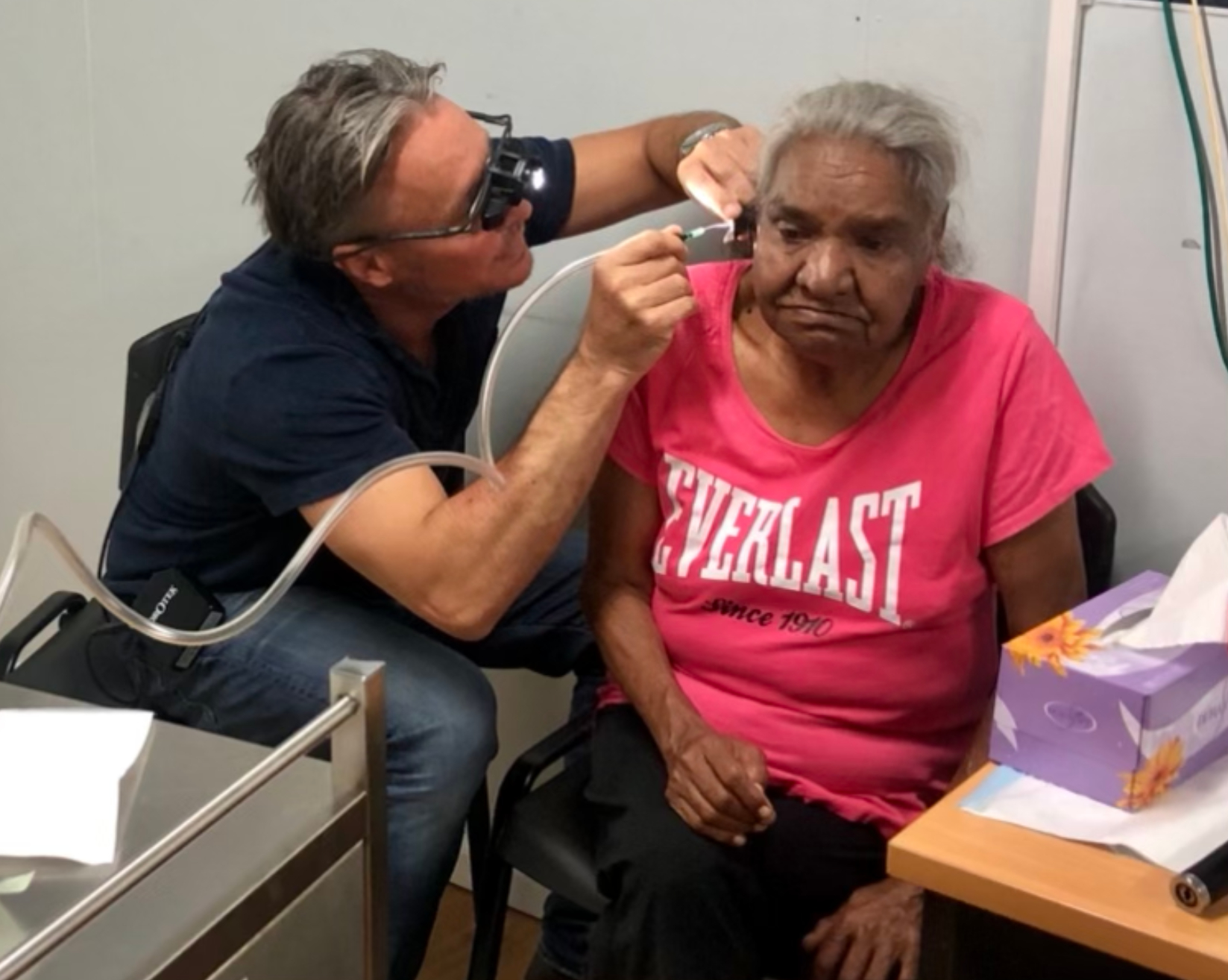
Dr William Mooney is actively involved in research, education and has presented and been widely published locally and internationally on the topic of Facial Plastic Surgery and rhinoplasty. Dr Mooney has worked extensively in the public hospital system and philanthropic work is important to him, especially with regard to indigenous health. He has made over 50 trips to a clinic in Darwin, NT which serviced indigenous Australians as well as service men and women and local Darwinians. He is has been a sitting member of NICENT advisory sub-committee to OHNS, RACS board, and is involved in outreach medicine to rural communities in NSW.
Only trust your care to a fully qualified surgeon who has obtained a fellowship from the Royal Australasian College of Surgeons. Always ask your surgeon about their experience and formal training in your planned procedure.
[mpc_carousel_image preset=”default” single_scroll=”true” loop=”true” auto_slide=”true” delay=”1000″ speed=”500″ images=”230,2972,3230,3228,3224″ rows=”1″ cols=”1″ gap=”0″ start_at=”1″ image_size=”full” image_opacity=”100″ image_border_divider=”true” image_hover_opacity=”100″]
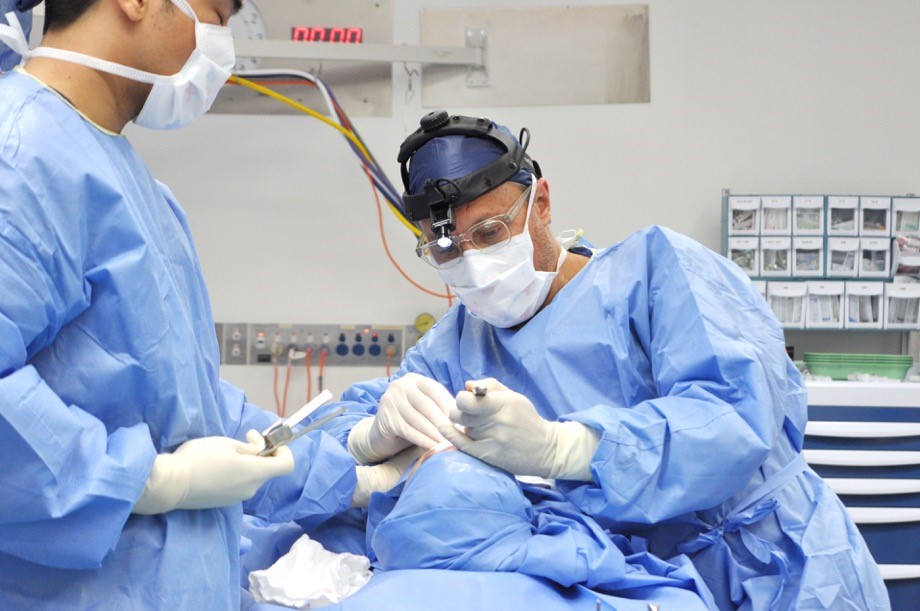
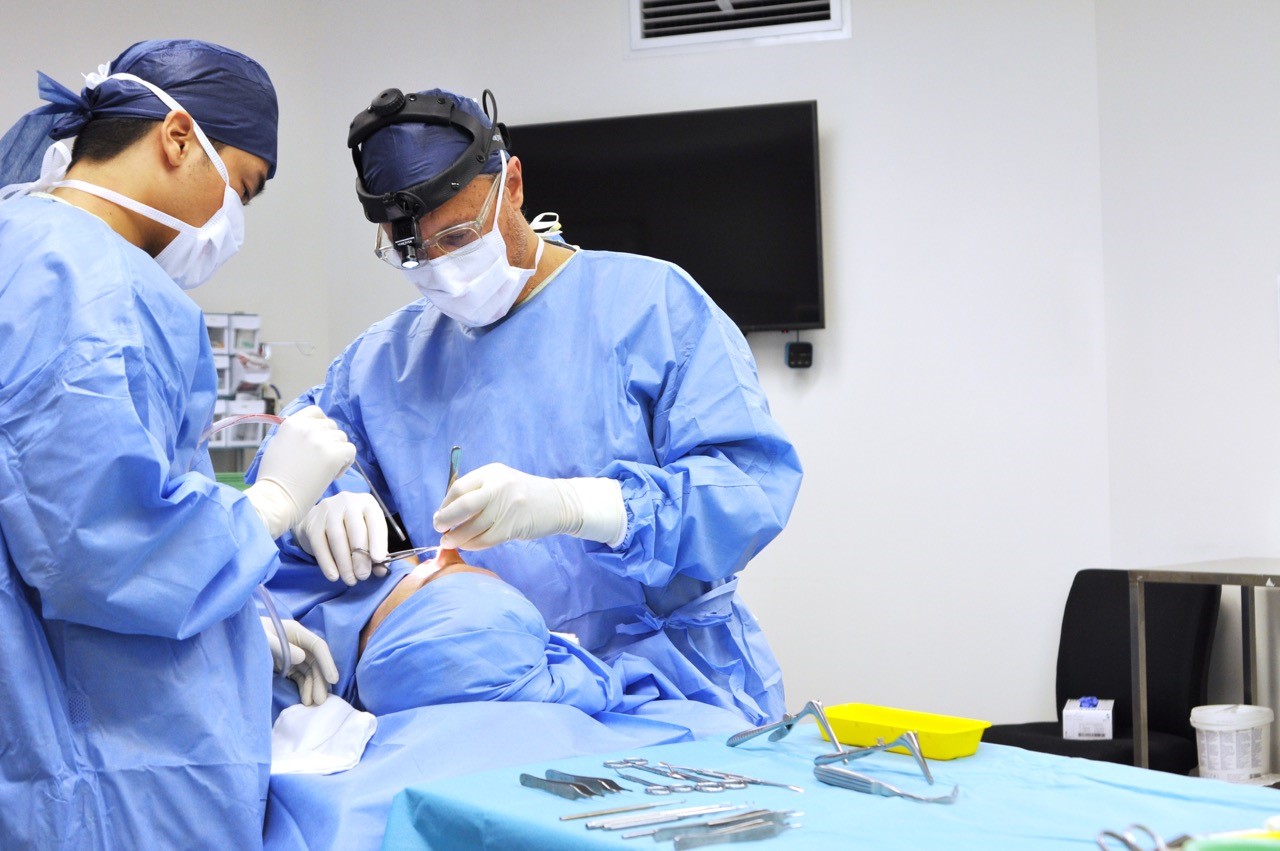
Dr William Mooney is a senior, experienced Ear, Nose and Throat Surgeon specialising in Rhinoplasty and Facial Cosmetic Surgery.
Dr William Mooney began his career at a most interesting time in medical history. Advances in technology were beginning to have an incredible impact on how we could operate upon and medically treat our patients. Dr Mooney began as a general surgeon but decided to specialise in Ear, Nose & Throat (ENT) surgery. From there he always had a plan to focus his career on head and neck cancer surgery and Rhinology.
After Dr Mooney set up practice he found himself seeing many nasal presentations and realised as well as correcting the external shape of the nose, addressing breathing issues was also important. At this point in time rhinoplasty nose surgery in Australia was still in its infancy.
Cosmetic surgery garners criticism from some quarters. Dr Mooney often says he feels those critics should walk in the shoes of some of his patients. Often they have issues, especially nasal problems, as a result of unwanted and significant trauma.
Whether Dr Mooney is correcting a sporting injury or addressing a person’s cosmetic concerns, it’s an enormous responsibility and challenge. He finds such a great joy being an ENT surgeon and working on reconstructing such important areas of a person’s face.
It takes decades to develop the skills required for this delicate work. One of his many mentors and teachers, Professor Bridger made an enormous impact on his life. The Prof’ used to say…
“In the first part of your career you learn how to operate, then you learn when to operate, then you learn when not to operate.”
DR WILLIAM MOONEY’S BACKGROUND
Dr Mooney says he was interested in medicine for as long as he can remember. He came from a medical background. His father was a wonderful, highly respected and accomplished paediatric ENT Surgeon. He was head of the ENT department at the Royal Children’s Hospital in Melbourne for 20 years. Dr Mooney senior was an innovator and introduced the first laser to ENT surgery in Australia in 1973. He used it to treat Laryngeal Papillomatosis, lesions in the voice box, that can kill children. It’s a terrible complaint; one particular child required 112 operations– every time effectively saving this boy’s life! Dr Mooney calls his dad an inspiration, although the first time he took a young William into an operating theatre, aged 11, he fainted!
In HSC Dr Mooney topped the state in Latin, which later would make anatomy, where so many names are in Latin, much easier.
DR WILLIAM MOONEY’S MEDICAL TRAINING
Medical school took six years, with 40 hours of lectures each week. Dr Mooney chose Monash University because, at the time, he says he felt it was the more progressive of the two Melbourne Universities. He graduated in 1990 and won the Medical prize and the Surgical prize in his final year.
Then came hospital residency, a total of six years at the Alfred Hospital in Melbourne. Although Dr Mooney tried many specialities, he kept being drawn back to ENT. William remembers being simply fascinated with the depth and breadth of the specialty. It covered areas such as Neurosurgery, paediatrics, laryngology, head and neck cancer oncology as well as of course Rhinoplasty and Facial Plastic Surgery.
The only other speciality Dr Mooney was interested in was plastic surgery. However, it was a very different era to now, as the only plastic surgery he saw in the public hospitals was amputations, burn victims and other traumas. About the only elective cosmetic surgery was Otoplasty(ear), Rhinoplasty(nose) and Breast Augmentation, and in those days, was not commonly performed, nor was it taught in detail.
When Dr William Mooney decided to officially specialise in ENT Surgery, he joined the four-year intensive training program in NSW. His first placement was at John Hunter Teaching Hospital in Newcastle. This was an incredible hospital with an enormous throughput of surgeries, allowing him to really hone his skills on a variety of procedures from Paediatrics to incredibly delicate laryngeal (voice box) operations. In his training Dr Mooney worked at some of the leading hospitals in the country including Prince of Wales and Prince Alfred. At the end of these four years, he qualified as an ENT surgeon, but prior to setting up private practice Dr Mooney made the decision to focus his future work on Rhinology and Head and Neck Cancer.

SHADOWING LEADERS IN THE FIELD
After being awarded his fellowship, Dr William Mooney spent six months at the Australasian Academy of Facial Plastic Surgery in Sydney. This was critical to learn how to run a practice as most ENT surgeons have a combined private practice and public hospital appointments.
Then to London to work under two specialists famed in their fields.
David Howard (Past President of the British Laryngological Association), is one of the most renowned head and neck cancer surgeons, anywhere. Howard was very calm, steady and deliberate. Dr Mooney says Howard taught him an invaluable technique to ensure each operative step progressed the surgery forward in order to advance the operation. This was critical learning. William often says it taught him to operate calmly, effectively and always with purpose.
Professor Valerie Lund is Professor of Rhinology at the Ear Institute, University College London and is an Honorary Consultant ENT Surgeon at the Royal National Throat Nose and Ear Hospital (University College London Trust), Moorfields Eye Hospital, and University College Hospital. She is considered one of the greatest rhinologists in the world. She taught Dr Mooney the delicacy of the nose and the value of a more restrained approach – the balance of surgery and medicine. She probably operated on about one in eight of her rhinology patients, treating many of the others with medications and a conservative technique.
In Paris Dr William Mooney worked with Jean Abitol who at the time was the voice guru. He introduced him to the intricacies of the larynx (voice box) and the micro instruments required. He also taught Dr Mooney the importance of the connection between psychology and laryngology: the important interplay between the voice and the mental health of his patients. Over time, Dr Mooney believes he has extrapolated this learning to emphasise the importance of mind and body on all his patients. We now live in a time where we commonly see body dysmorphia, which is the anxiety around one’s appearance. This was his first insight into how important the stability of the mind is to the health of my patients.
In New York Dr Mooney spent time with Jatin P. Shah, known as the ‘Godfather’ of head and neck cancer surgery, at the Memorial Sloan Kettering Cancer Centre, the leading cancer centre in the world.
Then to the Lasky Clinic in Beverly Hills, which is focused on Rhinology and cosmetic facial surgery for the stars. Dr Mooney says he found LA was a different world! Up until this time was a rhinoplasty surgical technique called the Goldman Tip (reconstruction of the nose tip), which is fast and looks good, but long-term has problems. William always says it was an important lesson in what not to do. Dr Mooney still fixes a lot of Goldman Tips to this day. Also, many of his patients were African Americans who wanted to reduce the width of their nostrils. Interestingly Dr Mooney wasn’t happy with the techniques being used as dark skin often scars significantly, so he developed an internal scarless alar base reduction technique, which he uses to this day.
BACK IN AUSTRALIA
Initially Dr William Mooney worked in Melbourne with his Dad. Then in 2003 he was invited to join the practice of one of his surgical mentors, Professor Bridger, a head and neck cancer surgeon. It was a fortuitous decision because of the cultural diversity in western Sydney, as Dr Mooney reports learning a huge skill set. He was exposed to nose patients of both sexes, with a great deal of trauma, sporting violence, reduction rhinoplasty, augmentation rhinoplasty, alar base reduction, and more.
Five years later Dr Mooney extended his practice to Bondi Junction. He now has 33 years of diverse experience as a practising doctor and 22 years as an ENT Surgeon.
Dr Mooney always says he loves his work. Rhinoplasty, whether to fix a sporting injury, or other significant trauma can be a most intricate procedure as it combines the treatment of both function and form, a delicate balance between addressing nasal breathing and the contour of the nose.

LOOKING AHEAD
Dr William Mooney plans to continue operating and performing surgery on my two main passions; Rhinology and Head and Neck Cancer Surgery.
Also very important to him is his philanthropic work, cancer and general work in the public sector, and my involvement in indigenous health and an outreach program with clinic visits to rural communities in NSW.
He has been an active member of NICENT (The First Nations ENT society), attending their meetings, is involved in research and has attended remote clinics frequenty.
Research has always been important to Dr Mooney, and as well as presentations for NICENT he is working on projects in Sydney. In the last two years he has set up several new research projects, gathering data on what Dr Mooney calls the new ‘frontiers’ in modern medicine. He is also refining a Plasma-cartilage graft for rhinoplasty. He is also interested in the relationship between nasal obstruction and mental health which he often says he feels is a very real thing.
Dr William Mooney often describes his chosen profession is both challenging and extremely rewarding. Rhinoplasty, in particular, is constantly evolving to produce better outcome, making it efficacious and beneficial to his patients.
This is an exciting medial sector where one never stops learning and growing. In April, 2018 while lecturing at the Rhinology conference in Perth (hosted by the Australian Academy of Facial Plastic Surgery) William says he was humbled by the array of talent and forward thinking by his peers. Australia really is at the forefront of best practice in the field of Rhinoplasty. Dr Mooney believes is is an honour to be operating among the top echelons of surgeons.
In 2016 through his Bankstown clinic (and in association with Bankstown police and social services) Dr Mooney set up a pro-bono domestic violence facial trauma clinic. Often these victims had suffered trauma, fractured noses, facial scarring that couldn’t be treated in the Public Hospital system. At the same time their scars served as a constant reminder of the often horrific trauma they had suffered. The clinic was designed to help people who had in effect fallen through the cracks of the health care system. Dr Mooney will continue this work in his new clinics.
A huge advancement for the cosmetic industry is more thoroughly assessing the overall health of the patient, especially mental health prior to surgery. We now place a huge importance on lifestyle, naturopathy and the human psyche. Accommodating these holistic factors represents new thinking for traditional medicine and I am convinced they yield better long-term results for our patients.
Dr Mooney believes we are living in an era of extraordinary scientific advancements. We now use better materials, better medicines and better anaesthetic techniques. These medical improvements help us care for our patients and achieve better results long term.
We are also moving away from conventional surgical techniques and developing less invasive, in clinic, injectable options. The younger generations are dictating this demand for better product, for less, with immediate results. While these cost-effective alternatives won’t always replace surgery, they fill a critical gap in the cosmetic market.
As a father of two children, Dr Mooney is often nostalgic about his own upbringing and the incredible impact his father’s career had on his career choices. He says he always impresses upon them the things he has learnt: to be honest, meticulous and perform any task to the best of their ability. Whatever careers they choose, if they carry these motifs, he believes they will lead successful and honourable lives.
INDIGENOUS OUTREACH WITH DR WILLIAM MOONEY
Dr Mooney first attended regional indigenous communities as a surgical trainee flying to remote communities like Brewarrina in far Western New South Wales. During this time, he also attended a weekly indigenous outpatient clinic in Redfern. After his Fellowship, Dr Mooney travelled to the Northern Territory 50 times in 15 years.
He established a clinic in Darwin which had a significant Indigenous patients throughput. He also travelled to Tennent Creek and Katherine during this time.
Dr Mooney has been involved in the NICENT (National Indigenous Coordination of ENT Surgeons) committee which involved frequent meetings, research and visits to regional communities and clinics. He regularly visited clinics in Forster and Taree, as well as Tamworth and Inverell.

Ear disease is a significant issue for indigenous children as it further disadvantages them in many aspects of their life. Deafness associated with recurrent infections can make school a challenge. Early active treatment of ear disease can make a massive difference in the lives of these patients.
Dr William Mooney is passionate about helping these communities and plans to remain active in the service of these Australians. (informed consent for photography of Indigenous Australians is always gained for image inclusion)